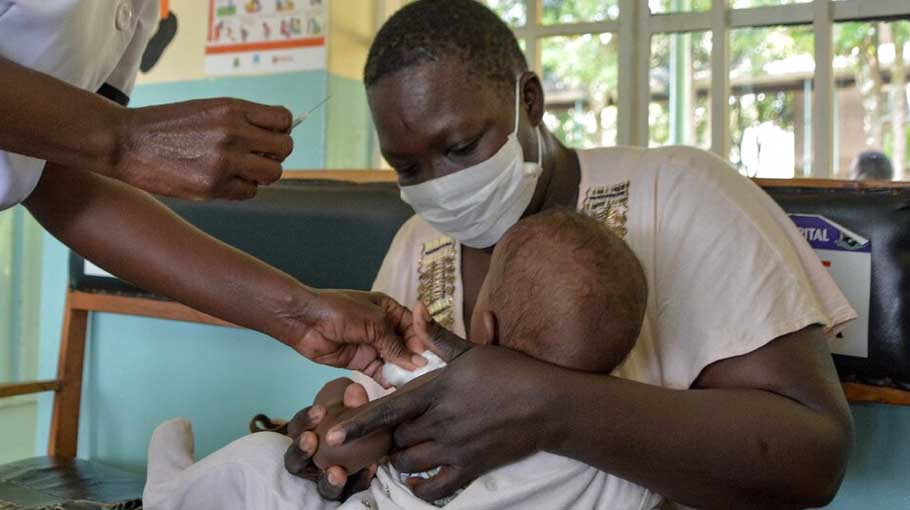
What the Malaria vaccine means for Africa

Like many who work in public health, especially in sub-Saharan Africa, I’ve been waiting my whole career for a malaria vaccine. And even longer than that: I suffered from severe malaria when I was 10.
The World Health Organization has now endorsed the first vaccine as a complementary tool for widespread use among children in at-risk areas, including my country, Senegal. This announcement, hailed as “historic” by the WHO and global health experts worldwide, is indeed cause for celebration. Malaria is a preventable disease that has been virtually eliminated in wealthy countries and yet kills around 400,000 people a year, mostly African children.
While this is a watershed moment for global health, the vaccine — called Mosquirix — has modest efficacy, preventing about 30 percent of severe malaria cases. It’s not perfect and will not be a miracle solution.
To save the most lives, countries must stay invested in scaling up teams of local health workers to respond to cases and increase access to the right set of tools such as mosquito nets and antimalarial drugs for preventing the disease. The new vaccine is an important proof of concept, and is paving the way for the next generation of potentially more effective malaria vaccines using a variety of technologies, like mRNA, which is used for some Covid-19 vaccines.
It has taken a generation to develop the first-ever malaria vaccine
thanks to political commitment and financial support from many
partners. With more investments and effective tools, we can be the
generation that will end the disease for good
Inspired in part by my own experience with malaria and disparities I have seen in getting treatment, I founded a nonprofit, Speak Up Africa, 10 years ago to champion solutions that are developed in Africa to address public health challenges facing the continent. Malaria is at the top of the list, as it has arguably the greatest impact on African nations’ economic and social development. But other endemic illnesses — often grouped as neglected tropical diseases — are no less debilitating and in need of greater research and development investments.
Africa must be at the heart of these investments. The continent is a fertile ground for innovation in health care and beyond, and I am convinced more solutions to fight malaria and other deadly diseases will emerge from here. Continued efforts and support — such as financial and technical assistance to increase local lab capacity for research — are critical.
Countries need strong health systems that can deliver the best prevention tools, including vaccines. This includes investing in hundreds of thousands of additional community health workers who can go door-to-door in remote and rural communities to more quickly detect, diagnose, treat and report malaria cases and other diseases.
The new malaria vaccine will be most successful if it’s a complement to other measures, such as mosquito nets, antimalarial drugs and the indoor spraying of houses. African countries also need access to high-quality epidemiological data to understand where people are most at risk for infections, where insecticide and drug resistance is taking hold, and which tools are working best in local communities. This can allow for more tailored and effective malaria interventions.
This milestone in the global malaria fight should also spur further investment in additional malaria vaccines already in the pipeline to ensure a healthy market, but also in other much-needed new tools such as genomic surveillance to stay one step ahead of growing drug and insecticide resistance.
Covid-19 has taught the world that vaccine manufacturing in Africa must be expanded to end the current pandemic and prevent future ones. Currently, Africa imports 99 percent of its vaccines.
A new African Medicines Agency, under the African Union, is set to launch in November with the goal of improving safety regulation of medical products in the continent. I am hopeful that regulatory pathways will be established to accelerate the development and uptake of safe and effective health products — including vaccines.
My country, Senegal, is being considered as a potential manufacturing hub by the Covid-19 vaccine maker BioNTech for future mRNA vaccines against not only Covid-19, but also malaria and tuberculosis. Along with HIV/AIDS, these are still the continent’s biggest killers. More investments into African scientists and institutions are needed if the world wants to gain the upper hand on deadly diseases.
It has taken a generation to develop the first-ever malaria vaccine thanks to political commitment and financial support from many partners. With more investments and effective tools, we can be the generation that will end the disease for good.
Yacine Djibo is the founder and executive director of Speak Up Africa, a nonprofit based in Dakar, Senegal, focused on public health and development in Africa.
Source: The New York Times.